
Closing Report — Community Options, Inc.
Table of Contents
- Posted on - 02/25/2026
BY ELECTRONIC, OVERNIGHT, AND REGULAR MAIL
Re: Closing Report — Community Options, Inc.
Dear Mr. Sweeney:
As part of its oversight of the New Jersey Medicaid program (Medicaid), the New Jersey Office of the State Comptroller, Medicaid Fraud Division (OSC) conducted a limited-scope audit to determine whether Community Options, Inc. (Community Options) complied with applicable Medicaid requirements for services it provided at a group home in Parsippany (Parsippany Home) during the period January 1, 2024 through December 31, 2024 (audit period), and how it allocated Medicaid funds it received during the audit period. OSC has completed its review and hereby issues this Closing Report.
OSC did not find any material deficiencies regarding Community Options’ operations of the Parsippany Home, which houses four Medicaid beneficiaries. OSC reaches this conclusion after having reviewed, among other things, Medicaid beneficiaries’ daily service notes, direct care employee timesheets and payroll records, background checks and training records, incident reports, and personal funds statements. As explained more fully below, OSC does note that from the Medicaid funds it received, Community Options allocated approximately 40 percent to its net profit and administrative expenses, which greatly exceeds the 12 percent that a state consultant had recommended for use as a benchmark for the state’s group home rate-setting in 2014.[1] This means that for the Parsippany Home, Community Options allocated more than three times the dollar amount of Medicaid funds to its own profits and administrative expenses than envisioned by state rate-setting consultants.
Audit Objective
The objective of this audit was to determine whether Community Options operated the Parsippany Home in conformity with applicable state and federal statutes, regulations, and guidance, particularly those outlined in the Community Care Program Policy Manual (CCP Policy Manual). In addition, OSC reviewed Community Options’ allocation of New Jersey Medicaid revenue, both for its New Jersey operations overall and for this specific location, across direct care, ancillary, and administrative or profit costs, and compared these allocations to the proportions modeled in the state’s 2014 group home rate-setting study.
Audit Scope
The scope of this audit covered the period from January 1, 2024 through December 31, 2024. However, for detailed testing, OSC selected a judgmental sample covering the period of October 1, 2024 through October 31, 2024, focusing on the Parsippany Home, which is one of the 138 group homes operated by Community Options in New Jersey. This audit was conducted pursuant to OSC’s authority as set forth in N.J.S.A. 52:15C-23 and the Medicaid Program Integrity and Protection Act, N.J.S.A. 30:4D-53 to -64.
This was a limited scope audit and, as such, the results described herein should not be interpreted as representing Community Options’ overall compliance status with Medicaid requirements. Rather, the audit was designed to provide a limited review of service delivery, documentation practices, and allocations of Medicaid revenue related to both Community Options’ New Jersey operations, totaling approximately $78 million annually, and the Parsippany home, totaling approximately $953,000 annually. This review does not constitute a full operational or financial examination of Community Options’ Medicaid-related activities.
Audit Methodology
To accomplish the audit objective, OSC reviewed applicable regulations set forth in N.J.A.C. 10:44A, the CCP Policy Manual, and the Community Options Operation Manual.
OSC performed an on-site visit of the Parsippany Home and conducted interviews with Community Options personnel to gain an understanding of the organization’s operations, internal controls and processes, as well as specific procedures related to the Parsippany Home.
For detailed testing, OSC evaluated whether Community Options provided and properly documented the contracted daily services it billed under Healthcare Common Procedure Coding System (HCPCS) H2016 (Comprehensive community support services, per diem) during a sampled review period of October 1, 2024 through October 31, 2024 (sampled review period). OSC reviewed documentation including beneficiaries’ daily service notes, employee timesheets and payroll records, direct care staff employment and training records, and incident reports to assess compliance with applicable state regulations and the guidance established in the CCP Policy Manual. In addition, OSC reviewed beneficiaries’ statements of personal funds to verify that these records were properly maintained and that no indications of personal fund mismanagement were identified.
Finally, OSC obtained and analyzed Community Options’ revenue/expenses for calendar year 2024 both at the corporate level related to New Jersey Medicaid and for the Parsippany Home, and compared the information contained in these documents to relevant Medicaid program information, including rate-setting guidance.
Background
Overview of Group Homes in New Jersey
Group homes in New Jersey are regulated by the Division of Developmental Disabilities (DDD) within the Department of Human Services (DHS), under N.J.A.C. 10:44A and the CCP Policy Manual. The Office of Program Integrity and Accountability within DDD conducts inspections and investigations of these homes to ensure they meet health, safety, and regulatory requirements. DDD’s oversight focuses on adherence to Home and Community Based Supports rules, provider monitoring, and the quality of services delivered to beneficiaries.
A group home is one type of licensed residential setting under DDD’s Community Care Program. The program provides housing, meals, personal guidance or training, and community integration for eligible Medicaid beneficiaries, depending on the beneficiaries’ required level of care. Group homes are owned or leased by licensed providers, and typically operate in private houses or apartments staffed by direct care employees. Group home staff provide supervision, training, assistance, and other services to support beneficiaries’ daily living activities. In general, Medicaid pays group home providers a daily rate (per diem) using payment tiers based on each beneficiary’s assessed needs. Moreover, in addition to this per diem payment, the group home provider receives additional funds from Social Security and other payers that are applied toward rent and food, and other costs. Finally, the Medicaid program pays day treatment providers separately for services provided to DDD group home residents who receive care in these settings.
The New Jersey Medicaid program annually spends approximately $2 billion on group home-related services. Of this amount, Medicaid paid 133 group home providers approximately $1.6 billion in calendar year 2024 for services billed under HCPCS H2016 (Comprehensive Community Support Services per diem), which cover daily residential supports provided to 9,649 Medicaid beneficiaries residing in group homes. The remaining amount, approximately $400 million, reflects payments for other residential and related services billed by group homes and other providers under additional HCPCS codes, including H2016 (Comprehensive Community Support Services, per 15 minutes), T1002 (Registered Nurse Services, up to 15 minutes), T1003 (Licensed Practical Nurse Services up to 15 minutes), and T1019 (Personal Care Services per 15 minutes) serving an estimated 14,462 eligible individuals.
Overview of Community Options
Community Options, Inc. is a national non-profit organization incorporated in 1989 in New Jersey. Community Options primarily provides residential housing through group homes and supervised apartments for individuals with developmental and intellectual disabilities such as Autism Spectrum Disorder, Cerebral Palsy, Down syndrome, or physical disabilities, traumatic brain injury, and dual diagnoses. In general, Community Options offers group home residents assistance with daily living activities, healthcare coordination, transportation, and recreational programming. Additionally, the organization provides vocational training and access to therapeutic services to address the needs of individuals with behavioral challenges.
According to its website, Community Options operates in many other states, including Arizona, Iowa, Maryland, New Hampshire, New Mexico, New York, Pennsylvania, South Carolina, Tennessee, Texas, and Utah.[2] Nationally, Community Options provides residential and employment supports to over 6,700 people with disabilities and manages more than 700 group homes[3], with 138 of those homes servicing 426[4] individuals in New Jersey.
Operation of Community Options’ Parsippany Home
For this audit, OSC selected as the test sample one of Community Options’ 138 group homes located in Parsippany, New Jersey. DHS Office of Licensing approved this group home for operation in September 2019. According to its latest license covering the OSC audit period, the Parsippany Home is approved to provide services for four individuals.
The direct care staff at the Parsippany Home was responsible for assisting beneficiaries with daily routines such as cleaning, cooking, feeding, medication administration, and personal hygiene. They also monitored health and medical needs, supported the development of independent living skills, and facilitated community participation through activities and appointments. Additionally, staff was responsible for maintaining accurate and timely program documentation. Community Options assigned to the Parsippany Home a total of 11 direct care staff, including a house manager, on a rotating basis during the sampled review period. On average, two direct care staff were present during the morning and evening shifts when beneficiaries were in the home, while typically only the house manager was present during the day, when beneficiaries attended a day habilitation program outside of the home.[5]
Direct care staff primarily was responsible for providing daily living services between 3:00 pm and 9:00 am, which includes overnight supervision of beneficiaries. During the day, beneficiaries attend a day habilitation program for which Medicaid separately reimburses contracted providers. Direct care staff was responsible for ensuring that beneficiaries were ready in the morning to attend the day program. Staff also confirmed that each beneficiary boarded the transportation van and was received off the van upon return in the afternoon. In some cases, direct care staff personally transported beneficiaries to and from the day care program, as needed.
Audit Observations
A. Documentation and Billing Requirements
OSC reviewed Community Options’ documentation, including Medicaid beneficiaries’ daily service notes, direct care employee timesheets and payroll records, background checks and training records, and incident reports, to determine whether Community Options’ documentation satisfied the requirements set forth in N.J.A.C. 10:44A and the CCP Policy Manual.
OSC found that Community Options’ documentation adequately supported the daily services billed to Medicaid under HCPCS H2016 (Comprehensive community support services, per diem), during the sampled review period. In addition, OSC reviewed employment records for direct care staff who served Medicaid beneficiaries during the audit period, and determined that Community Options properly screened these employees prior to hire and the employees satisfied the required training.
Based on its findings, OSC is reasonably assured that Community Options complied with the relevant documentation and billing requirements during the sampled review period.
B. Use of Beneficiaries’ Personal Funds
OSC reviewed the beneficiaries’ personal funds accounts for calendar year 2024 to determine whether Community Options properly managed and documented these funds. The review included statements of personal funds and supporting documentation for transactions recorded in each beneficiary’s account.
OSC found that Community Options generally maintained adequate documentation to substantiate expenses and appropriately used beneficiaries’ personal funds for individual needs such as clothing, hygiene products, and recreational activities, including group meals and community outings. Community Options’ records also reflected instances in which the organization temporarily advanced funds to beneficiaries when account balances were low, with corresponding repayments documented in the account statements. Overall, OSC did not identify any issues indicating mismanagement or inappropriate use of beneficiaries’ funds.
C. Allocation of Medicaid Funds toward General Administrative Expenses/Profits
As stated above, the New Jersey Medicaid program paid approximately $1.6 billion to 133 group home providers in calendar year 2024 for HCPCS H2016 alone. Of that $1.6 billion, Community Options received approximately $78 million for providing services to approximately 426 Medicaid beneficiaries who resided across 138 of its group homes in New Jersey.
For calendar year 2024, OSC found that both at the local level (Parsippany Home) and statewide, for all of its group home operations in New Jersey, Community Options spent about 60 percent of its Medicaid revenue on direct care staff salaries/benefits and retained about 40 percent for administrative/overhead/profit. For the Parsippany Home for calendar year 2024, OSC found that Medicaid paid Community Options approximately $953,000. Of this amount, Community Options paid approximately $540,000 (57 percent) to direct care staff in wages and benefits. Of the remaining amount, approximately $413,000 (43 percent), Community Options spent $245,000 (25 percent) on administrative expenses such as management, vehicle costs, and overhead, and retained the rest, $168,000 (18 percent), as profit.[6] See Figure 1 below.
Figure 1: Major Expense Categories for Sampled Group Home (Parsippany Home)
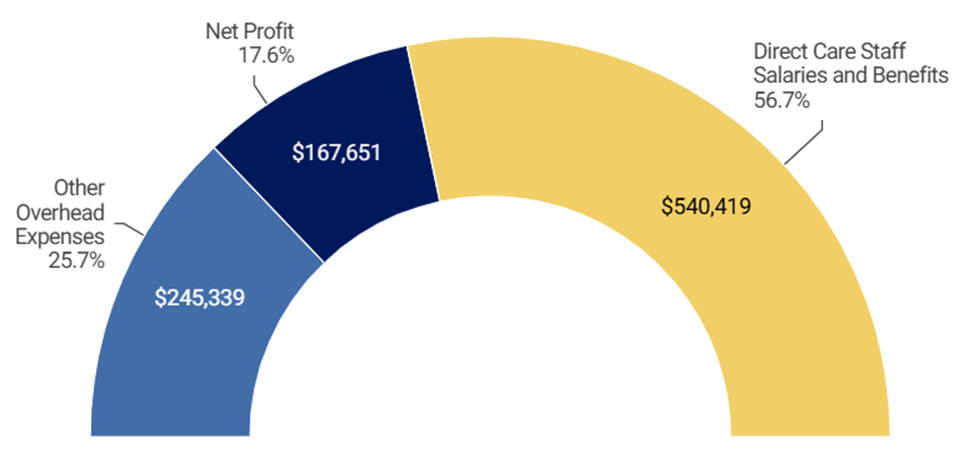
At the statewide level, for calendar year 2024, Community Options’ revenue/expenses breakdown is similar to the Parsippany Home. From the total amount of Medicaid funds Community Options received in the audit period, approximately $78 million, it paid approximately $48 million (61 percent) to direct care staff in wages and benefits and retained the remaining $30 million (39 percent). Of the amount it retained, Community Options spent $22 million (29 percent) for administrative and operating costs and retained the rest, $8 million (10 percent), as profit.[7] See Figure 2 below.
Figure 2: Community Option's Major Expense Categories for New Jersey
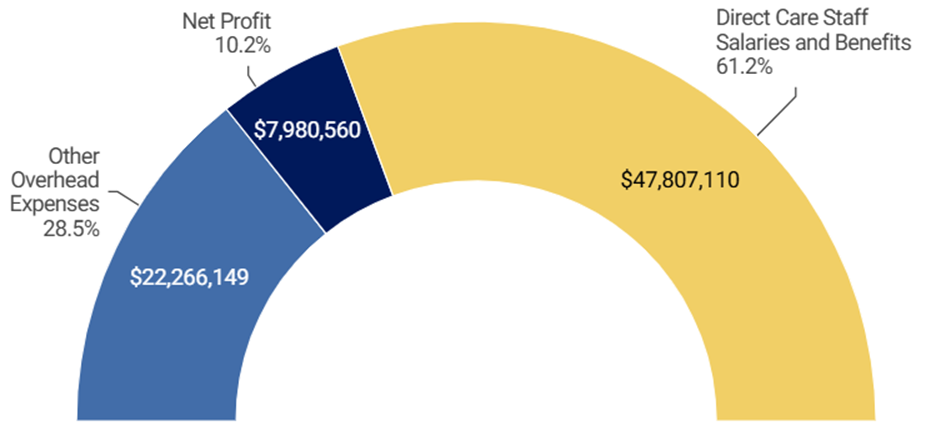
OSC notes these financially related findings regarding the breakdown of revenue between direct care costs and administrative/profits as observations, not adverse findings. There are no proscribed limits on how Medicaid funds are allocated between direct care and administrative costs/profits. The local and statewide analysis above shows that Community Options applied approximately 60 percent of its Medicaid revenue to direct care staff costs and retained the remainder, approximately 40 percent, for administrative expenses/profits. That breakdown, although not impermissible, allocates more than three times the percentage of Medicaid payments for administrative expenses/profits than the 12 percent that state consultants contemplated in 2014 when they provided a plan to state government officials to establish group home per diem rates.
Conclusion
For the reasons outlined above, OSC is closing this audit without any adverse findings. Accordingly, Community Options does not need to take any corrective action at this time. OSC’s decision to close this audit is based on its limited-scope review of services provided to Medicaid beneficiaries residing in the Parsippany Home during the period of October 1, 2024 through October 31, 2024.
OSC reserves the right to audit the Parsippany Home and/or other group homes operated by Community Options for the same or other periods to determine whether the provider complied with state and federal laws, regulations, and guidance.
Thank you for your attention to this matter.
Sincerely,
SHIRLEY U. EMEHELU
ACTING STATE COMPTROLLER
By: Josh Lichtblau
Director, Medicaid Fraud Division
[1] The firm Johnston, Villegas-Grubbs and Associates, LLC prepared a rate-setting study for the state in 2014 that modeled administrative and profit costs at approximately 12 percent of total expenditures. While this percentage was used for rate construction purposes and is not a regulatory requirement, it provides a useful benchmark for understanding how provider cost allocations compare to the assumptions used in the state’s rate-setting methodology. JOHNSTON, VILLEGAS-GRUBBS AND ASSOCIATES, LLC FOR THE NEW JERSEY DIVISION OF DEVELOPMENTAL DISABILITIES, DEPARTMENT OF HUMAN SERVICES, RATE CONSTRUCTION FOR DEVELOPMENTAL DISABILITY SERVICES (July 2014) https://www.nj.gov/humanservices/ddd/documents/Documents%20for%20Web/JVGA%20NJ%20Final%20Report.pdf.
[2] COMMUNITY OPTIONS, INC., OUR OFFICES, https://www.comop.org/about-us/our-offices/.
[3] Community Options, Inc., Community Options Named Largest Nonprofit I/DD Service Provider, June 25, 2025, https://www.comop.org/community-options-named-largest-nonprofit-i-dd-service-provider/.
[4] OFFICE OF PROGRAM INTEGRITY AND ACCOUNTABILITY, DEPARTMENT OF HUMAN SERVICES, DHS LICENSED REPORT CARD, REPORT ON DATA COLLECTED BETWEEN JULY 1, 2024 AND JUNE 30, 2025 (2025) https://www.nj.gov/humanservices/staff/opia/documents/Final%20DHS%20RM%20Report%20Card_7-1-2024%20to%206-30-2025.pdf.
[5] Daily living assistance for Medicaid beneficiaries residing in the Parsippany Home was provided in three shifts: morning (7:00 am to 3:00 pm), evening (3:00 pm to 11:00 pm), and overnight (11:00 pm to 7 am).
[6] Community Options did not provide a breakdown of Medicaid and non-Medicaid expenses on the income statement it provided to OSC. OSC recalculated Medicaid expenses in proportion to Medicaid revenue to calculate Medicaid costs for each expense category.
[7] See footnote 6.
Waste or Abuse
Report Fraud
Waste or Abuse
 Official Site of The State of New Jersey
Official Site of The State of New Jersey
