Please check this page often for updates and how you can prepare.
The federal government has changed the rules around who is eligible for NJ FamilyCare starting Fall 2026. These rule changes are part of the “One Big Beautiful Bill Act” that was signed into law by President Trump in July 2025. These new rules do not apply to everyone. The following information explains which members may be affected and how they can prepare.
What rules are changing & when?
Beginning October 1, 2026:
- Some non-citizen immigrants may no longer qualify for NJ FamilyCare.
Beginning January 1, 2027:
- Certain adults aged 19 to 64 will have to work, volunteer, or go to school to keep their coverage or qualify for NJ FamilyCare. This is called “community engagement.” These members must also renew their coverage every 6 months (instead of every 12 months).
- Other adults aged 19 to 64 may be exempt from the requirement to work, volunteer, or go to school, but they may still have to renew their coverage every 6 months.
NJ FamilyCare will contact you by Fall 2026 with more information if these changes apply to you. The new rules may affect your coverage starting on the dates listed below.
October 1, 2026
Some non-citizen immigrants may no longer qualify for NJ FamilyCare/Medicaid.
| Non-citizens who may continue to qualify include: | Non-citizens who may NOT continue to qualify include: |
|---|---|
|
If you are in one of these groups and have adjusted to Lawful Permanent Resident status, you may still qualify – please see more details below. |
| Non-citizens who may continue to qualify include: | Non-citizens who may NOT continue to qualify include: |
|---|---|
|
|
January 1, 2027
Certain adults will have to work, volunteer, or go to school to keep their coverage or qualify for NJ FamilyCare/Medicaid. These members must also renew their coverage every 6 months (instead of every 12 months).
Many members may not have to work, volunteer, or go to school, but they may still have to renew their coverage every 6 months.
Starting in 2027, NJ FamilyCare will check these requirements when you apply or renew your coverage.
Do I have to work, volunteer, or go to school?
| You may have to work, volunteer, or go to school if any of the following describe you: | You may NOT have to work, volunteer, or go to school if any of the following describe you: |
|---|---|
See below for how to check your plan type. What this means: If this describes you, you may need to work, volunteer, or go to school to qualify for coverage. NJ FamilyCare may ask you to provide documents showing proof of employment, volunteer work, or enrollment in a higher education or vocational program. |
What this means: If this describes you, you may not need to work, volunteer, or go to school to qualify for coverage. NJ FamilyCare may ask you to provide documents that prove your status. |
Do I have to renew my coverage every 6 months?
| You may have to renew your coverage every 6 months if any of the following describe you: | You may NOT have to renew your coverage every 6 months if any of the following describe you: |
|---|---|
See below for how to check your plan type. |
|
Please check this page often for updates on federal changes. Update your contact information so you do not miss important messages.
Where do I check/find my plan type?
- Call the member services number on the back of your current health plan ID card.
- Check the front of your health plan ID card – see below for instructions:
- If you are enrolled in Aetna, you will not be able to use this method. Please call the member services number on your health plan ID card.
- If you are enrolled in Fidelis Care, UnitedHealthcare, Horizon, or Wellpoint, please review the example Alternative Benefit Plan (ABP) ID cards below. If it says ABP or Alternative Benefit Plan on your card, as shown in the red boxes in the examples, you are enrolled in the ABP plan.

Fidelis Care
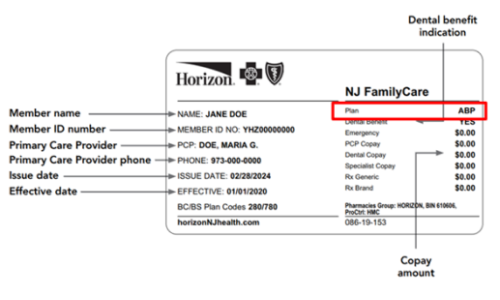
Horizon
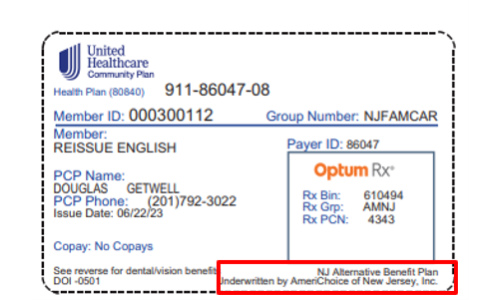
United Healthcare

Wellpoint
How is NJ FamilyCare/Medicaid helping members?
NJ FamilyCare is working to maintain health coverage and care for all eligible New Jersey residents. To manage the changes and share information with you, NJ FamilyCare is partnering with State agencies, providers, health plans, advocates, and other groups. In addition, NJ FamilyCare is investing in technology and improving its processes to make applying and renewing easier and more reliable.
When it’s time for you to renew, NJ FamilyCare will review your information to see if your coverage can continue automatically.
- If NJ FamilyCare already has the information it needs, you will receive a letter telling you your coverage has been renewed.
- If NJ FamilyCare needs more information, you will receive a request for information letter or renewal packet. Please respond as soon as possible to avoid a gap in coverage.
How can you prepare for changes?
- Use the NJ FamilyCare Activity Requirements Checker and find out in 10 minutes if you will need to meet the new requirements.
- Keep using your NJ FamilyCare benefits and go to your appointments.
- Update your contact information so you do not miss important messages. Call NJ FamilyCare Customer Service at 1-800-701-0710 (TTY: 711) if your address or phone number has changed.
- Watch for letters, emails, or texts from NJ FamilyCare or your health plan.
- Open and respond to all mail from NJ FamilyCare as soon as possible.
- Apply or renew your coverage even if you think you may no longer qualify.
- Check this website often. NJ FamilyCare will share more details as they become available.
This page was updated on February 17, 2026.
 Official Site of The State of New Jersey
Official Site of The State of New Jersey